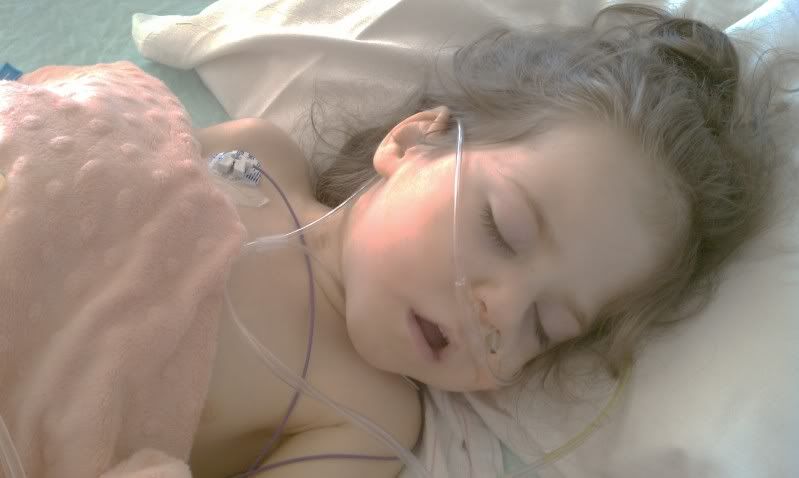
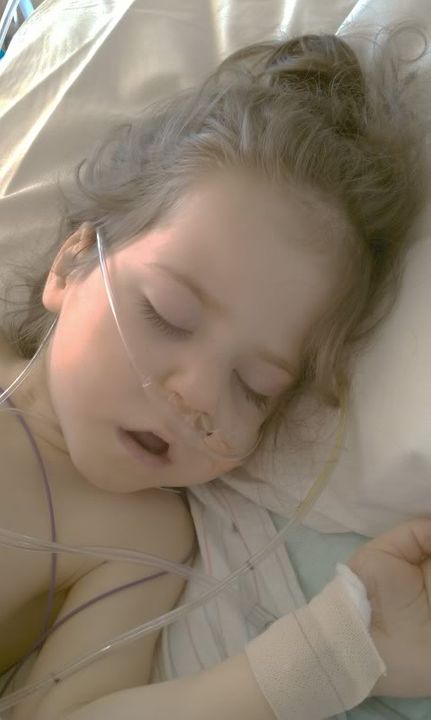
Ella did not sleep much last night. She was fighting sleep till 2:30am. Then with all the nurse and doctor visits, she only got a few hours. But she was in as good of a place as we could have expected for this procedure.
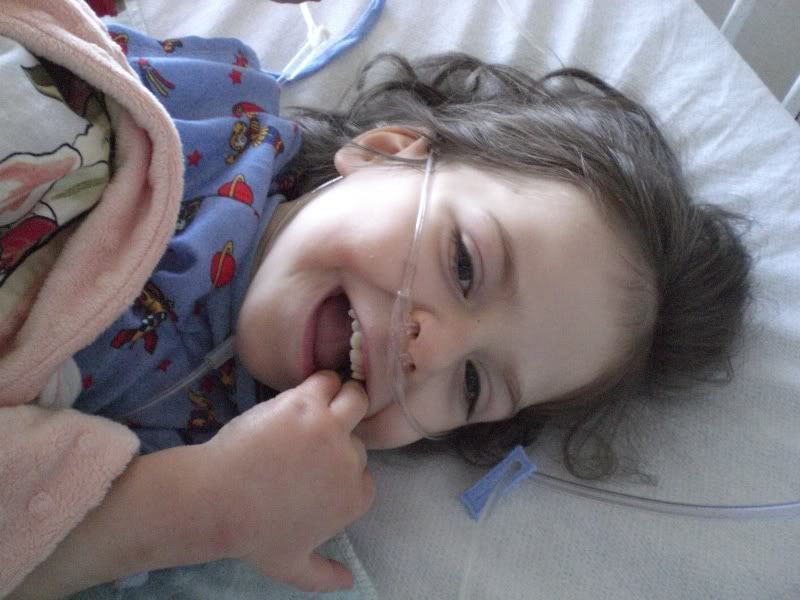
About 9:15am, they transported her downstairs to the OR room. We were in the pre surgery area, talking with the anesthesiologists and surgeon.
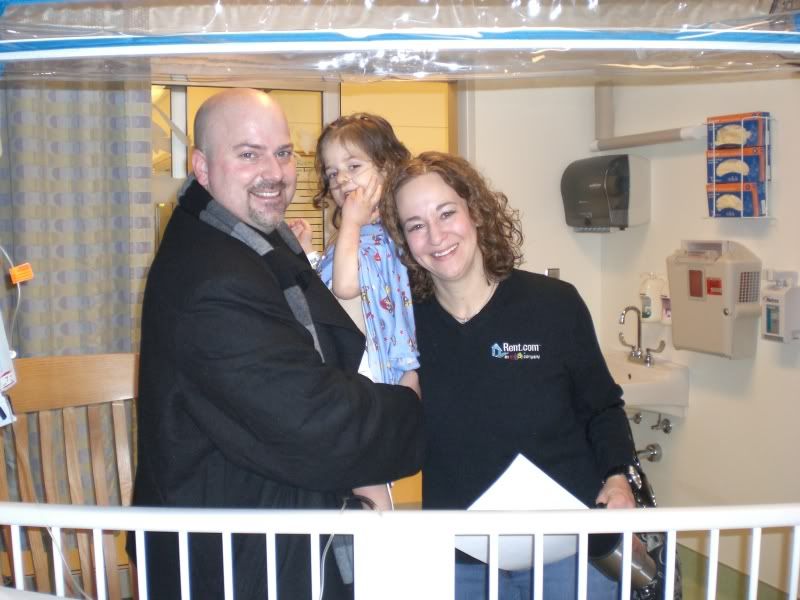
We went over all of our concerns including how they planned to manage her pain. We did not want the same issues that we encountered in CA with her last surgery and heavy dosing of narcotics. It is so reassuring though – the team here is great. They really listen to parents.
Afterwards, we dressed for the OR complete with suits, masks and hair nets so we could walk back and be with Ella as they put her to sleep.
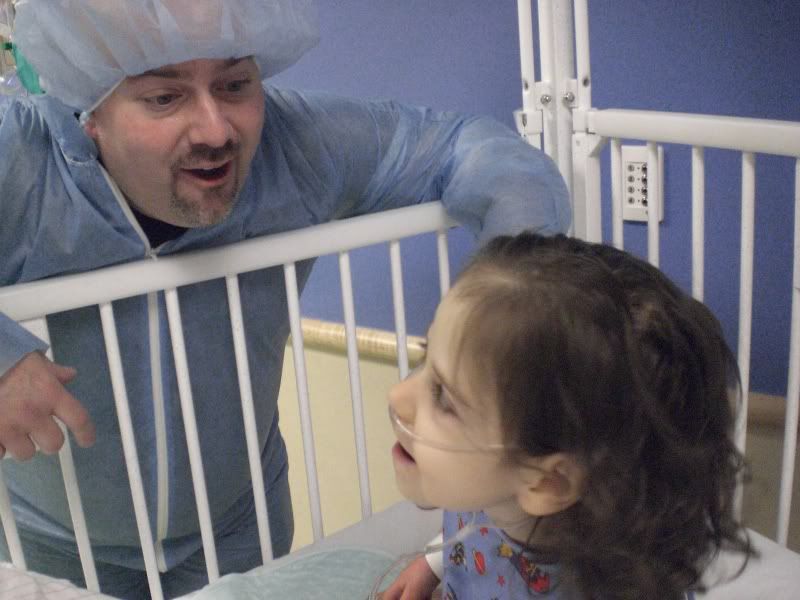


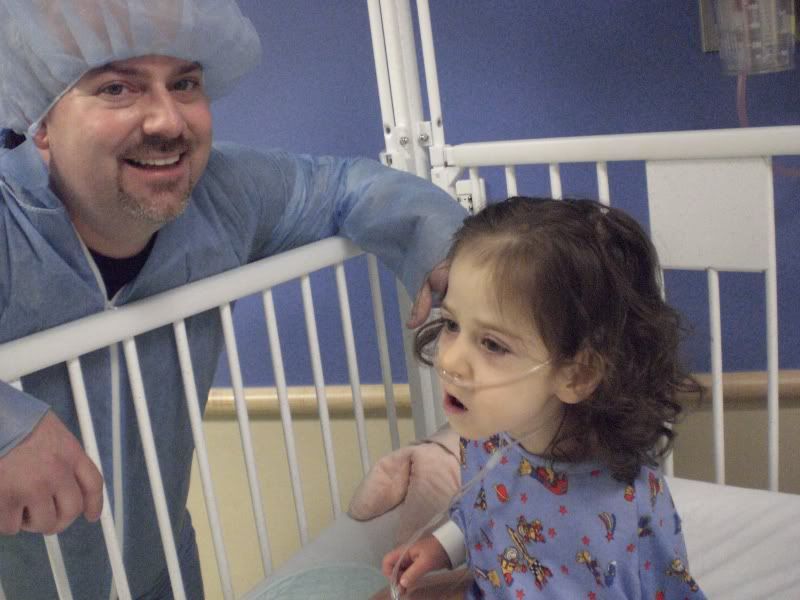

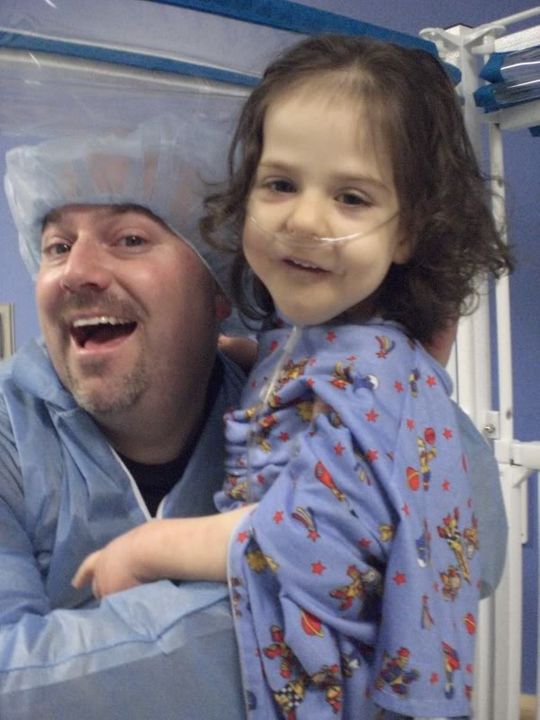
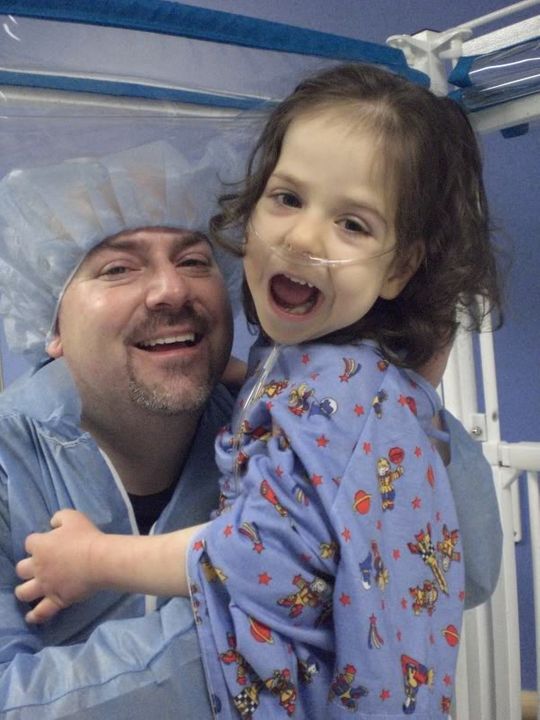
They gave her Versed via IV first which made her loopy and smiley. Then, they administered Propofol to put her to sleep. Before they administered the heavy anesthesia, Josh asked if we could take a moment to pray over our child. Of course, I expected the humble moment before God to cause some tears. What I did not expect: the anesthesiologist asked for one moment to finish a task so that he could pray with us. We held hands and surrendered our child to the Lord.
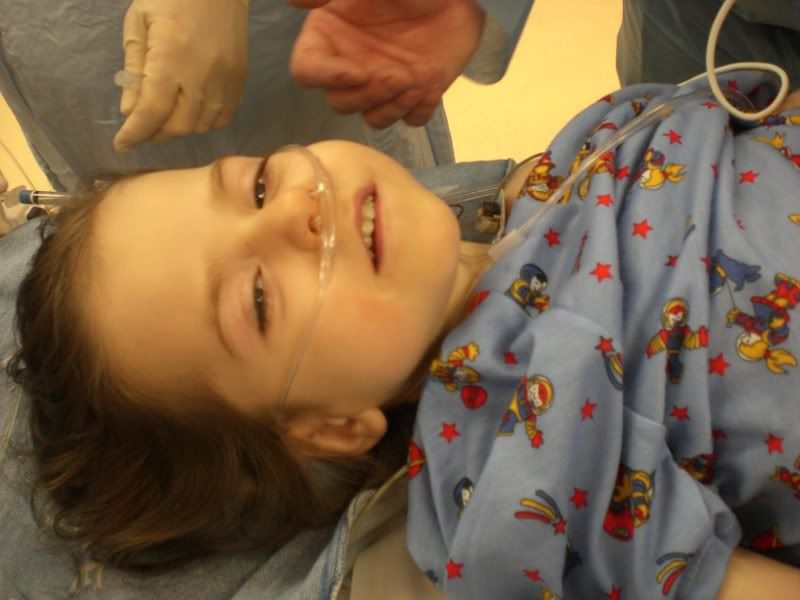
UPDATE by Tina at 10:50am MST: At 10am, we walked out and surgery was officially started. They just called at 10:50am, to give us an update that Ella is doing fine and that Dr. Partrick just made the first incision. Thanks for all the thoughts and prayers.
UPDATE by Tina at 12:15am MST: The nurse just called from the OR. Dr. Partrick did have to use more gortex patch to repair the diaphragm hernia. Ella is still stable and they are getting ready to close. Likely another 45 mins to an hour before its complete. Everything has gone smoothly so far.
UPDATE by Tina at 3:45am MST: We went back to the recovery area to see Ella. Wow, it doesn’t get any easier…it’s just hard to watch your child go through these procedures. Fortunately, she was extubated – that is HUGE. If you remember during her last surgery at CHOC, they did not extubate her and then had to dose her with narcotics to keep her sedated. Here, they extubated her and she is stable on 2 liters of O2 via her cannulas.
We spoke with Dr. Partrick (surgeon) and he said that everything went well. There was a significant hole in her diaphragm and most of her colon was in her chest. He had to use another gortex patch about 3cm x 5cm to cover up the new hole. He noted that her nissen and hiatal hernia repairs from previous procedures still looked intact. One thing that did surprise him was the amount of scar tissue/adhesions in the chest cavity. The colon had not just floated up to her chest, but had adhered with scar tissue to her lung tissue and surrounding areas. This is not common to see. So most of the surgery was removal of adhesions. In discussing it with him, one possible reason for more adhesions is because Ella’s chest cavity was scarred intentionally with betadine when she was in the NICU.
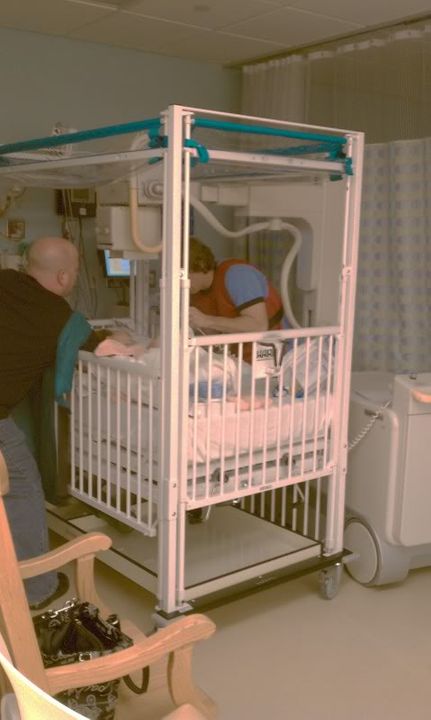
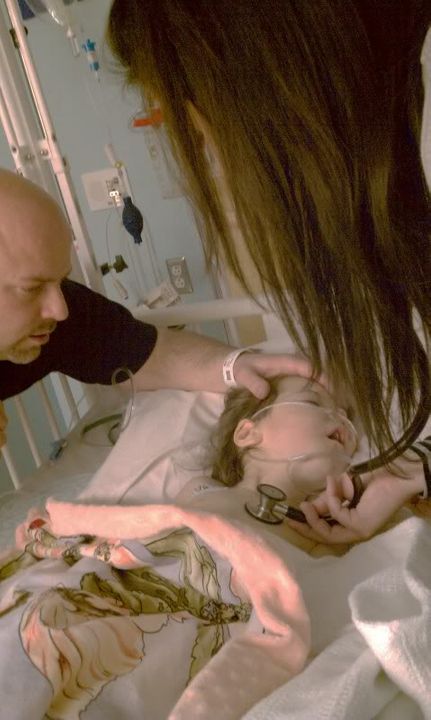
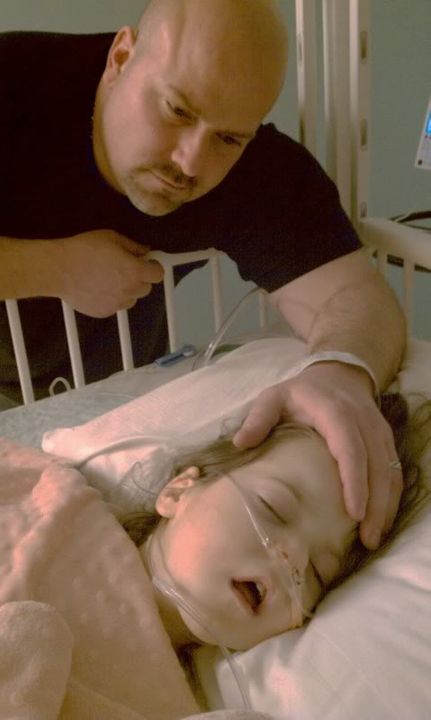
Although he cannot be 100% sure that this was the core cause of her recent pass out spells, he noted that the repair was more extensive than anticipated and was definitely impacting her pulmonary status and her GI system. All of us including the docs are hoping that once she recovers, we will not see any pass out spells.
The recovery nurse informed us that we were going to be put under the cardiac service. Once again, it required some advocating and intervening – Ella belongs under the pulmonary service. In this way, we were able to come back upstairs to the same room as last night.
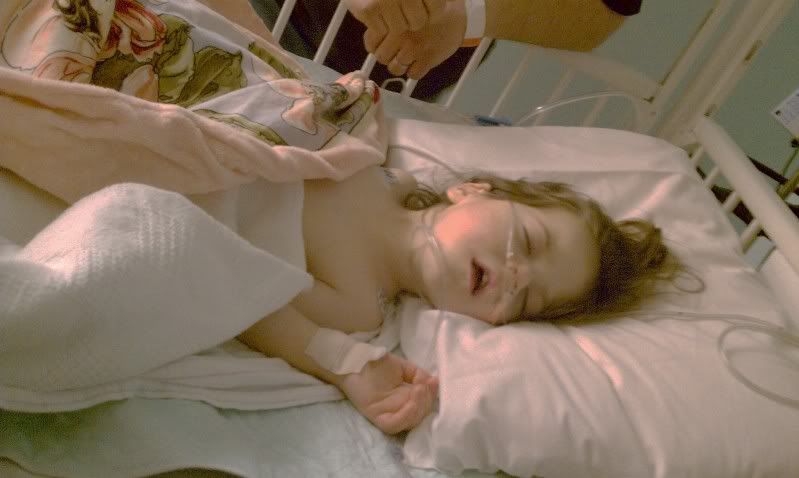
Right now, the plan is to keep her comfy with pain meds via IV (Dilaudid/Hydromorphone). If we think Ella is getting uncomfortable, we can push a button and administer more meds. They did give her one dose of morphine in the recovery area, but we’re trying not to use it since Ella gets itchy and can hurt herself with her fierce scratching.
She’s had decent urine output, but the pulmonary team is watching to see if they need to give her Lasix via IV. The plan is to keep her even with her ins/outs and stay on top of it through the night. We saw a chest xray – it looks a little hazy, but not bad considering everything. The surgery team is holding her food for 2-3 days and just letting her recuperate. If tonight goes well, we may be re-starting her plavix and aspirin to help with her SVC occlusion as early as tomorrow. She has a foley catheter and the NG tube is weaved through her nose to help decompress her stomach area. Plus, her G-tube is being continuously vented too. Hoping we can get rid of those things soon.
Thank you for all your continued prayers for Ella Renae.