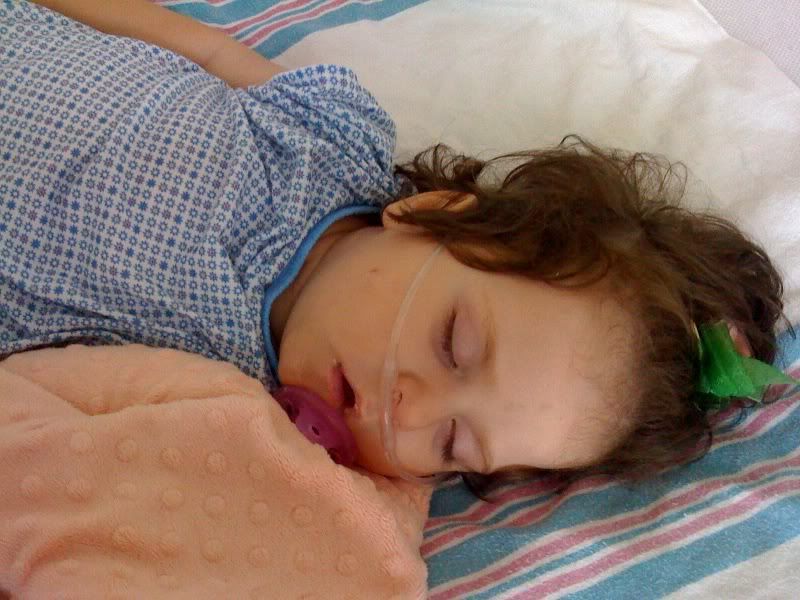
So, Ella remained stable overnight. The last dose of anti-itch medicine was later yesterday evening, but we have not had to use it since. As I type this at 10:45am, she is still asleep. We may need to use Atarax or Benadryl to control the itch once she is awake. She is still taking Methadone and Ativan for withdrawal symptoms, and receiving one of those meds every 3 hours. There may be discussion of reducing the dosage, but we’ll see.
She is still on the nitric oxide to control her pulmonary hypertension and sits at 2 liters. While she is asleep, her numbers look great most of the time. We’ll see when she is awake throughout the day. It was disheartening to see her wanting to be more alert and playful yesterday and her body not able to keep up with it, thus the nitric oxide.
Once again, I’m a bit frustrated about the fluid overload situation. As of late last night around 10pm, she was still 2 liters positive for the past 4 days and her weight was 15 kilos (she was 15.1 kilos the night before). Not really any change, so I went and asked the attending if we could increase the IV Lasix dose to once every 6 hours. As of this morning, she was not positive by a lot but still positive for a 24 hour period between 100-150. It’s not a huge amount and based on her weight, they consider that inconsequential. They told me that they are only concerned if she is 300+ positive for a 24 hour period. But once again, she is still 2 liters positive for the past 4 days and Ella is fluid sensitive and does not respond like a healthy 2 year old. Being positive at all when she is already fluid overloaded is not inconsequential!!! They took a look at her chest xray from this morning and it looks unchanged from yesterday. Ya think?
When I talked with the docs, it seems that they are not getting the picture about being aggressive and really drying her out. So, I called down to CHOC Medical Records to see if I could get a print out of all the written records since admission, so I can forward it to Denver. I want her pulmonologist to see how they are treating her pulmonary hypertension and this fluid situation. I want a second opinion. Plus, he knows how different Ella responds and just how dry she needs to be for her pulmonary system to function optimally. CHOC charges 25 cents per page to fax it over to Denver (ridiculous), but I’m going to take on the expense because I need a pulmonology expert to weigh in. Overall, CHOC has been great but they do not know Ella and continue to treat her with the same protocol as other patients AND they do not have any pulmonology experts (Denver has 18 – it is a speciality for them). All we did yesterday was give her enough Lasix to maintain her in the same place. They are not being aggressive enough and treating her pulmonary status in a way that I am comfortable with – so – it’s time to get Denver more involved.
On a positive note, Ella seemed to tolerate her food at 10ml per hour just fine without any discomfort. So, surgery would like to increase her rate to 20ml today and try it. However, they are waiting to see if Ella will stool. Her last bowel movement was Sunday afternoon. She has been taking her home regiment of Miralax for the past few days. So if she doesn’t stool on her own soon, they will look to give a suppository later today and want to see another stool before letting her increase on her rate of food.
In the meantime, I’m advocating and ruffling feathers in the PICU. I guess it’s my role in life. Sigh…
Psalm 68:19
Praise be to the Lord, to God our Savior,
who daily bears our burdens.

