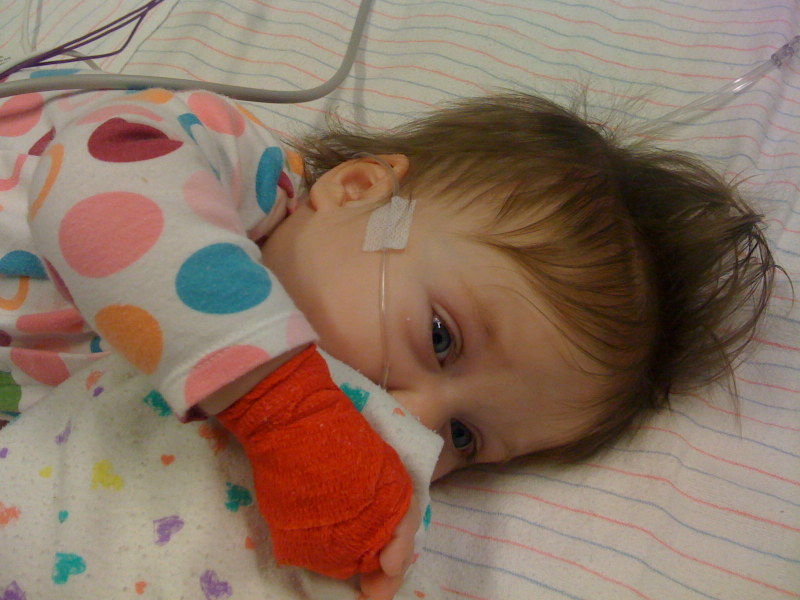
Ella was wheeled down to the cath lab at 11am this morning. The procedure itself didn’t get started until around 12:20pm. Tina was able to go into the room with her while the anesthesiologist put her to sleep with some gas.
The doctor performing the heart cath mentioned that he may want to balloon open some veins (possibly her SVC) and could potentially use a stent to keep it open.
I just received a call (1:20pm) from the nurse practitioner letting me know that they were able to get access right away (Praise God!) and they were already testing the pressures in her heart.
At the moment, Tina and I are both outside soaking in the beautiful weather. I’m here escaping into work and she’s taking some alone time to make some calls.
We’ll post updates as the details come in from the procedure. Thank you for continuing to lift us all up in prayer.
Thank you Jesus for this beautiful day. We praise you for the gift of life, and the miracles you’ve performed in the hearts of many through our precious daughter. We ask that you give revelation to the doctors through this procedure, enabling them to more effectively treat our girl. Father, keep her safe. We pray for no complications and for stability during and after the procedure. We completely surrender and trust in you Lord. Praise you Jesus. Amen.
UPDATE 5:45pm MST (by Tina):
Ella was been stable throughout her entire procedure – praise God. She was in the procedure for about 4 hours. As Josh stated before, they had no problem getting access through her right leg. They weaved the catheter up to her heart and began to test the pressures and look at the anatomy of her heart and lungs.
The good news is that most of the major concerns with her heart were alleviated. The pressures in the different chambers were not normal, but not nearly as bad as they expected. They did confirm her pulmonary hypertension is moderate and on the arterial side. They feel that the sildenafil and captopril medicines play a huge role in keeping her stable.
Also, they were looking for 2 other potential major problems: narrowing/blockage of the veins in her lungs – those were not present. Her right lung looks good and although her left lung is smaller, both appear to be functionally working. Both have evidence of chronic lung disease with some abnormalities, but there was no narrowing of the veins coming from the lungs into the heart. Another concern was the pressures in her heart. Yet, when they gave her nitric oxide and more oxygen, she responded favorably and the pressures came near to normal.
They’ve confirmed that her SVC (superior vena cava) is completely occluded and cannot find veins on her right side going back into her heart. They are only able to see collateral veins that loop all over the right side of her body.
They were hoping that they might be able to get access in some way to the SVC so that they could try and balloon it open. They tried going into her right neck and her left neck, but did not have success at locating a place where they could balloon it open. When we looked at the images, literally there is no SVC going into Ella’s heart. The SVC is not just occluded; the opening to that part of her heart is closed off completely.
So doing the heart catheter certainly eliminated a lot of scary diagnosis that they thought she might have had going into the procedure. It told them which medicines are going to be the most effective in treating her. The plan for now is to increase her sildenafil dose to 6mg per kilo, three times per day to help with her pulmonary hypertension and increase the aldactazide diuretics to .75mg per kilo every 24 hours, divided into two doses. The plan is to watch her clinically and increase the meds as needed.
We are supposed to have another Care Conference soon to have everyone brainstorm about the best plan of action on a long term basis. Another thought: Dr. Fagan who did the procedure today took the time to show us all the images of the procedure. It was amazing to see the video clips of Ella’s heart, lung and collateral veins. Dr. Fagan thinks it might have more benefit than risk to schedule another heart catheter procedure to see if they can try to re-create the path from her heart through her SVC. If Ella’s body had that vessel open and provided another way to drain into her heart, it would likely relieve some of the pressure and it could be playing a huge role in her fluid sensitivity. If they could re-create the pathway of her SVC, they would likely place a stint to keep it open.
This is the same theory that Dr. Kays had about her fluid sensitivity. Back in Gainesville, he wanted us to consider the same type of procedure. However, the cardiology staff at Shands did not have an expertise for this type of procedure and they stressed how risky it would be for Ella, given her prognosis at the time. So, we held off.
Dr. Fagan can’t guarantee that he could get the path re-created, but he could try with minimal risk. If he does get the path re-created and places a stint, he can’t guarantee that it would resolve her problems. But on the other hand, it might. Something to consider for Ella.
The course for the next few days is to stay steady and play around with the same cocktail of medicines, trying to get Ella in a good place. I’m hoping that her Care Conference can be early next week and that we can talk about taking her home soon!
Thank you for the amazing outpouring of support and prayers. It meant so much to have people praying for all three of us today. We’re overwhelmed and overjoyed at everything He has done through this journey. We continue to trust and be in awe of the path He has chosen for us to follow.