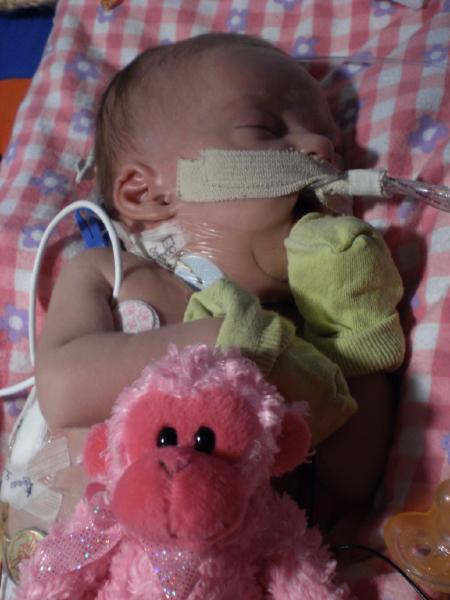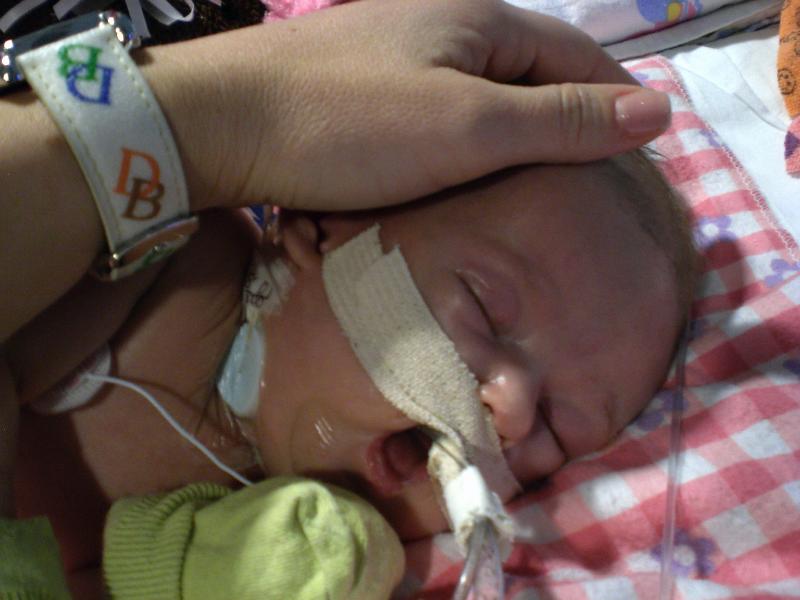
About 6:30pm, we met Dr. Kays at the hospital and talked about Ella’s next steps.
Dr. Kays told us why he wanted to proceed with replacing the left chest tube. He pulled up Ella’s latest chest x-ray from today to show us how much fluid was in her pleural cavity.
It was not a surprise. When we saw her tonight, you could tell that she was more puffy, was having a tough time breathing and did not feel well. Then, he showed us a chest x-ray from a few days ago – wow, what a difference!
Also, when we arrived her latest blood gases had gotten worse and there was no chest fluid coming from the right chest tube at all, yet you could tell that there was fluid in her chest from the x-ray.
So, one of the questions we asked him was why he decided to remove the left chest tube on Monday versus the right chest tube. Since Ella’s diaphragm was missing on the left side and there is a patch there from her repair surgery, the longer that the chest tube remains in her, the greater chance of infection.
We asked if he would use the same incision to re-insert the chest tube or if he would be performing a separate incision. He said that he was not sure until he was in surgery mode and looking at the existing incision. His gut instinct was that there is higher risk by using the same incision, but then again, he better feel strongly if he is going to insert a chest tube in a brand new location. He doesn’t just want to give her another scar on her side without good reason.
After a long discussion of her fluid issues and all of our options, the best option at this point was to re-insert the chest tube on her left side.
He mentioned that he wanted to replace the left chest tube, let her stabilize and then consider replacing the right chest tube late this week, if necessary.
Well, we got a call around 8:45pm and the chest tube procedure had been completed. Ella did fine during the procedure.
Dr. Kays is always thinking on his feet and surprising us: he decided to replace both chest tubes! After he thought about it more, he knew that there was fluid in her chest on the right side from her x-ray earlier and yet it was not draining (most likely due to a protein build up in the line). So, he opted to replace both chest tubes and luckily was able to use the same chest incisions.
When we called this evening at 11pm, already her fluids were beginning to drain. Praise God!
Just since the procedure was finished around 8pm, she has drained 62 total from both chest tubes. That is a big difference from zero over the prior 24 hour period. Also, her blood gas performed at 9pm shows that her body is getting happier, cO2=61, pO2=109. So, already we are seeing improvement. Thank goodness that Ella is getting some relief.
After we let her stabilize and wait patiently, we really need the fluid issue to resolve on its own. If it doesn’t, the only other options to explore are not real appealing.
We can have the SVC procedure completed again, where they open up her collapsed superior vena cava going into her heart. This operates under the assumption that the blockage or lack of flow into her superior vena cava is backing up, causing a leak of the lymph fluid out of her thoracic duct into her pleural cavity. Dr. Kays is not in favor of this route because the risks are high and we did not see any benefit from doing the procedure the last time.
After that, the only other option is to consider invasive surgery. This is a last resort and is only considered when you have tried all other therapies and the fluid issue is not resolving. It makes the assumption that the thoracic duct is damaged. Your thoracic duct is complex and is part of the lymphatic system which runs throughout various parts of your body. The surgery involves trying to locate a leak in her thoracic duct and repairing it. There could be a single leak or various leaks anywhere in the thoracic duct and there is not a way for them to locate the leaks with any precision. Therefore when surgery is performed, the success rate is not real high.
As you can probably tell, our hearts are heavy. We really want to see Ella overcome this fluid issue so she can move on to other milestones.
Please continue to pray for our baby girl. Our heart’s desire is to see the Lord heal this fluid issue miraculously. Ultimately, we know that He is in control and that we can trust His plan.
Hebrews 4:16
16 Let us therefore come boldly to the throne of grace, that we may obtain mercy and find grace to help in time of need.