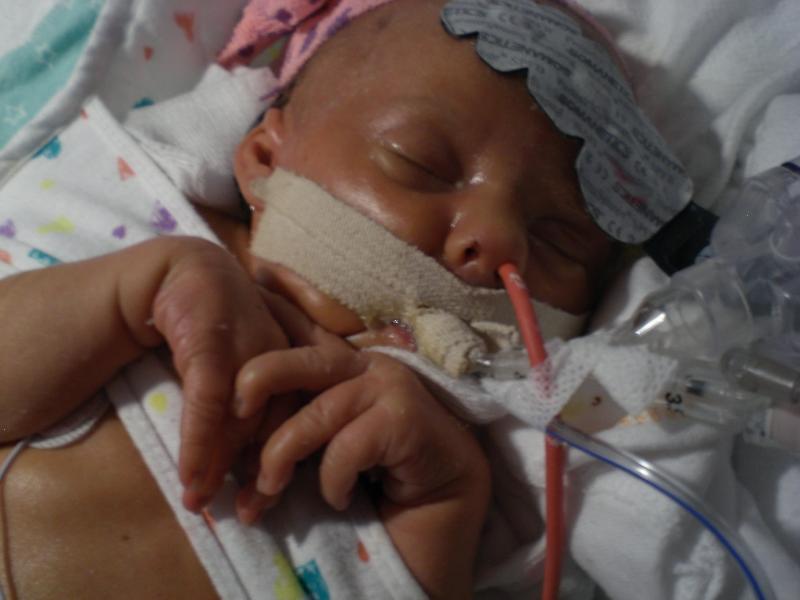
Praise Jesus from whom all blessings flow!
Today was a big day and our last update was an indication of how touchy the situation has been. Ella had a lot done today so hang on…there’s a lot to share.
We started out with an ECMO flow reduction to 60. Dr. Kays called this morning and said that if they can get a PICC line in they would attempt to remove her from ECMO this afternoon. Inserting a PICC line is not a trivial task and doesn’t always work the first time. Angie (one of the NICU III rock stars) was able to get the PICC line guided in on the first try! THANK YOU FOR THE PRAYERS!!!!
After Ella settled down, they started to take her off ECMO. We could not be in the NICU during the procedure. We had to wait, and pray (I think God had us right where He wanted us). Once she was stable, we were able to go in and see her. She looked good, but her stats were a bit unsteady. Dr. Kays was hovering over her like a concerned parent.
The one stat you can watch fluctuate moment by moment is her oxygen saturation level. It was hovering around 95. Dr. Kays wants to see a solid 100. But he indicated a 95 or better is ok. Her chest x-ray looks pretty good. Her right lung is looking almost fully inflated and her left lung has inflated a bit. Her heart has also shifted more towards the center of her chest.
We talked to him about where things might go from here. He described a few possible scenarios:
He indicated that if she makes significant progress, and her stats keep going up and stabilize, he will put off surgery for awhile. It is better to give her lungs more time to grow and for her to get stronger than to push surgery right away. I would have thought that all her organs up in her chest cavity would cause other stresses to the organs, but he indicated that he didn’t think so. The other advantage of waiting on surgery is to allow more of the fluids to be removed from her body, and for her heart and liver to recover.
If her stats just maintain without any real progress, he may look to do surgery sooner, hoping to give her lungs even more room.
But..
If her stats go the wrong direction, he may have to put her back on ECMO. We really don’t want this happen.
One of the challenges to this surgery is getting all her guts back into her belly and having enough space to do so. While on ECMO her liver can swell and her heart can too. This poses a problem of too much stuff trying to fit into too small of a space. If they absolutely had to, they could do the surgery in phases, but this is not a desired track. Hopefully we won’t have to go down that path. This is another reason to wait more before doing the surgery so that the swelling that does exist can go down as much as possible.
After discussing these things, Dr. Kays went around and tweaked a couple things and stood over her for awhile. He then checked in on a couple other patients and said goodbye to us for the evening.
We were there with Angie (the rock star PICC line nurse) and had our eyes on our baby girl. The staff had taken another blood gas and her cO2 (carbon dioxide) gases were high (59). They wanted to see that level around 40. We were also watching her oxygen saturation specifically, desiring to see it go up to 100 as Dr. Kays had hoped. It hovered around 95 for awhile, 96..95..96…95. Up to 96, then back down to 95….then to…94. A bit later 93…94…93, 92…91, 92. Oh man we’re going the wrong way and I can see the concern on Tina’s face. Tina went to go pump and when she got back…
90…89…90….88
The nurses paged Dr. Kays.
Tina indicated that she wasn’t able to express any milk and that we needed to get something to eat. I didn’t really want us to go, and I don’t think she did either. But Tina is trying to juggle taking antibiotics 4 times a day (1 hour before you eat or 3 hours after) while pumping every 3 hours and trying to eat enough to keep her milk production up. We hadn’t had anything to eat since breakfast and it was 2pm…we had to get some food. So, we left our girl in the NICU’s hands and hesitantly went to eat.
We were bummed. You know, we wanted instant gratification, but seeing the O2 number drop and the cO2 number increase was just a bit disheartening.
We ate our food and after about 30 minutes or so headed back to the NICU. We asked to go back in to see her but we were told we would have to wait for a nurse to come out and get us. So we waited. I only think we waited about 10 minutes but it felt like an hour. Angie came out and told us that she was doing ok, but Dr. Kays wanted her O2 levels to stabilize around 95 before he wanted us coming back in.
Tina decided to try and pump again and I waited to hear any news. Within 10 minutes Angie poked her head out and said that her levels were at 95 so it was ok to come in. Tina was still pumping so I headed back without her.
Dr. Kays was there and let me know that he had to use a dose of some medication to temporarily paralyze her, forcing her to calm down. He doesn’t like to use this technique unless he has to and it only works well because of the type of oscillating ventilator she’s on.
I went over to look at my baby. She was pretty still. Her eyes were twitching a bit. I asked if this was normal and Angie said that the medication was starting to wear off so I might see some movement. I talked to her for a bit and tried to comfort her. She started moving a bit more as time went on but her O2 saturation continued to hover around 95. Thank God.
After about 15 more minutes Tina came in. I stepped out of the way to let her get close to Ella. I sat off to the side and talked to another nurse. Tina was trying to comfort Ella when she fussed by putting her hands on her head and feet. This gives babies the impression of a confined space and Ella does pretty well with it. Tina noticed that when Ella calmed down and fell asleep, her stats would go higher.
We sat with nurse Angie for a couple hours until the shift change at 7:00pm. Parents are not allowed in the NICU during shift change so Tina and I stepped out for a bit. Tina went to go pump again and I updated the blog. After the shift change I went back in to see my baby girl.
I looked up at the O2 saturation level…
100
I waited…100…I waited three minutes…100. Her oxygen saturation level was pegged at 100 for three minutes! I just stood there…Ella sleeping…Daddy praying and praising our Heavenly Father.
For the next 10 minutes, her O2 level never dropped below 97. I told Tina I would come out after 15 mins, so I asked God to give me 100 just for a bit more. Her O2 level went to 100 for another solid minute. Thank you Jesus.
I talked to the night shift nurse for a bit. They had just completed another blood gas test. It indicated that her O2 levels were doing well, and her carbon dioxide levels had totally come back to where they should be (39)! This was a great ending to a big day for our little girl.
We pray that Ella sleeps well tonight and continues her positive track.
Thank you for your continued prayer support. God bless all of you!

Jeremiah 29:11 "For I know the plans I have for you," declares the LORD, "plans to prosper you and not to harm you, plans to give you hope and a future."
|
|
||||||||||||||||||||
|
|
|||||||||||||||||||||